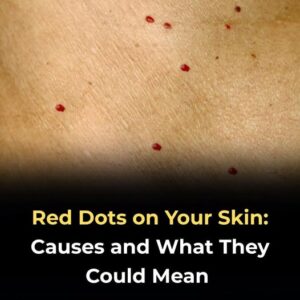
1. Cherry Angiomas (Most Common in Adults Over 30)
What They Are: Small, bright red, dome-shaped bumps caused by clusters of dilated blood vessels near the skin’s surface.
Why They Occur: Primarily genetics and aging. They are harmless, very common, and tend to increase in number as you get older.
Key Clue: They do not blanch (fade) when pressed. They are typically smooth, round, and range from pinpoint size to a few millimeters across.
Management: No treatment needed unless they bleed or bother you cosmetically. A dermatologist can remove them with laser or electrocautery if desired.
2. Petechiae (Tiny Broken Capillaries)
What They Are: Pinpoint red, purple, or brown dots that do not blanch when pressed. They result from tiny broken blood vessels (capillaries) under the skin.
Common Causes:
Vigorous coughing, vomiting, or straining
Sunburn or minor trauma
Certain medications (like aspirin, NSAIDs, or blood thinners)
Infections or immune responses
Warning: If petechiae appear suddenly, spread widely, or are accompanied by fever, fatigue, or unexplained bruising, seek medical attention promptly. These could signal an infection, clotting disorder, or other systemic issue.
3. Keratosis Pilaris (“Chicken Skin”)
What It Is: Rough, sandpaper-like bumps—often with redness around hair follicles—typically found on the upper arms, thighs, or cheeks.
Why It Occurs: A buildup of keratin (a skin protein) that blocks hair follicles. It is common, genetic, and harmless.
Key Clue: The texture feels like goosebumps or fine sandpaper. Redness may be more noticeable in fair skin.
Management: Gentle exfoliation and moisturizing with creams containing lactic acid, urea, or salicylic acid can improve texture. Consistency is key—results take weeks.
4. Heat Rash (Miliaria)
What It Is: Tiny red bumps or clear blisters that develop when sweat ducts become blocked, trapping perspiration under the skin.
Where It Appears: Chest, back, neck, and other areas prone to sweating or friction.
Key Clue: Occurs in hot, humid weather or after intense physical activity. May feel prickly or itchy.
Management: Cool the skin, wear loose breathable clothing, keep affected areas dry, and avoid heavy creams that can further block pores.
5. Allergic Reaction or Contact Dermatitis
What It Is: Red, itchy dots or patches that appear after skin contact with an irritant or allergen.
Common Triggers:
New laundry detergents or fabric softeners
Fragrances in soaps, lotions, or perfumes
Plants like poison ivy or oak
Metals such as nickel in jewelry
Skincare products with harsh ingredients
Key Clue: Itching is prominent. The rash often appears only where the skin touched the trigger.
Management: Identify and avoid the trigger. Use over-the-counter hydrocortisone cream for relief. Severe or persistent reactions warrant medical evaluation.
6. Insect Bites (Fleas, Mites, Mosquitoes, Bed Bugs)
What They Are: Small red dots, often in clusters or lines, sometimes with a central punctum (tiny bite mark).
Key Clue: Itching is common, especially at night (as with scabies) or after outdoor exposure. Bites may appear in patterns—bed bugs often leave linear clusters.
Management: Clean the area, apply anti-itch cream, and avoid scratching. If bites are widespread, persistent, or show signs of infection (increasing redness, warmth, pus), see a doctor.
7. Viral Exanthems (Viral Rashes)
What They Are: Red spots or rashes caused by viral infections.
Common Examples:
Hand, foot, and mouth disease: Small red spots or blisters on hands, feet, and mouth
Fifth disease: “Slapped cheek” facial rash with lacy red spots on the body
Shingles: Painful, blistering rash in a band-like pattern on one side of the body
Key Clue: Often accompanied by other viral symptoms like fever, fatigue, or sore throat.
Management: Most viral rashes resolve on their own with rest and supportive care. However, see a doctor if the rash is severe, painful, or if you have a weakened immune system.
8. Folliculitis
What It Is: Inflamed hair follicles appearing as red dots with pus-filled centers, resembling small pimples.
Causes: Bacterial infection (commonly Staphylococcus), yeast overgrowth, or irritation from shaving, tight clothing, or hot tubs.
Key Clue: Each red dot centers on a hair follicle. May be tender or itchy.
Management: Keep the area clean and dry. Avoid tight clothing and harsh shaving. Mild cases may resolve on their own; persistent cases may need topical or oral antibiotics prescribed by a doctor.
9. Autoimmune or Inflammatory Skin Conditions
What They Are: Red spots or patches resulting from the immune system mistakenly attacking healthy skin tissue.
Examples:
Lupus: Butterfly-shaped rash across cheeks or scattered red spots; may worsen with sun exposure
Psoriasis: Raised red plaques with silvery-white scales, often on elbows, knees, or scalp
Eczema (Atopic Dermatitis): Dry, itchy, inflamed red patches that may ooze or crust
Key Clue: These conditions are typically chronic, recurring, and may be accompanied by systemic symptoms like joint pain, fatigue, or fever.
Management: Requires medical diagnosis and a personalized treatment plan, which may include topical steroids, immunomodulators, or lifestyle adjustments.
10. Thrombocytopenia or Blood Disorders
What It Is: Easy bruising and petechiae (tiny red/purple dots) due to low platelet counts, which impair blood clotting.
Warning Signs:
Petechiae that appear without obvious cause
Frequent or unexplained bruising
Bleeding gums or frequent nosebleeds
Heavier-than-normal menstrual periods
Fatigue or weakness
Action Required: These symptoms require immediate medical evaluation. Blood tests can assess platelet levels and identify underlying causes.
11. Skin Cancer (Rare for Simple “Dots,” but Possible)
What to Look For:
A red spot that does not heal within a few weeks
A lesion that bleeds easily or crusts repeatedly
A spot that grows, changes shape, or develops irregular borders
A pimple-like bump that persists and does not respond to typical acne treatments (could indicate basal cell carcinoma)
Key Clue: Use the ABCDE rule for moles and spots: Asymmetry, Border irregularity, Color variation, Diameter larger than 6mm, Evolving changes.
Action Required: See a dermatologist promptly for any persistent, changing, or unusual skin lesion. Early detection is critical for successful treatment.
When to See a Doctor: Red Flags to Watch For
Consult a healthcare provider if red dots on your skin are:
Spreading rapidly across your body
Painful, oozing, crusted, or warm to the touch (signs of infection)
Accompanied by systemic symptoms like fever, fatigue, joint pain, or unexplained weight loss
Non-blanching: Use the “glass test”—press a clear glass firmly against the skin. If the redness remains visible through the glass, it may be petechiae and warrants evaluation.
Persistent: Lasting more than 2 weeks without improvement despite home care
Changing: Growing, changing color, or developing irregular borders
When in doubt, it is always better to seek professional advice. A dermatologist or primary care provider can offer accurate diagnosis and peace of mind.
Gentle Care Tips for Healthy Skin
While awaiting evaluation or managing benign causes, these practices support skin health:
Avoid Scratching: Scratching can break the skin, leading to infection or scarring. Trim nails short and use cold compresses to soothe itchiness.
Use Fragrance-Free Products: Choose gentle, hypoallergenic moisturizers and cleansers to minimize irritation.
Wear Loose, Breathable Clothing: Natural fibers like cotton allow skin to breathe and reduce friction.
Track Potential Triggers: Keep a simple journal noting new products, foods, activities, or environmental changes that coincide with skin changes.
Protect from Sun: Use broad-spectrum sunscreen daily. Some rashes worsen with sun exposure.
Stay Hydrated: Drinking adequate water supports overall skin health and barrier function.
Frequently Asked Questions
Q: How do I know if a red dot is serious?
A: Focus on accompanying symptoms. If red dots are painless, stable, and not accompanied by fever or other concerns, they are likely benign. Rapid changes, pain, or systemic symptoms warrant evaluation.
Q: Can stress cause red dots on skin?
A: Yes. Stress can trigger or worsen conditions like eczema, hives, or psoriasis. Managing stress through relaxation techniques may help improve skin symptoms.
Q: Are red dots from allergies contagious?
A: No. Allergic reactions and contact dermatitis are not contagious. However, some viral rashes or bacterial infections that cause red spots can be contagious—practice good hygiene if infection is suspected.
Q: Can I pop or squeeze red dots like pimples?
A: No. Popping can introduce bacteria, cause scarring, or worsen inflammation. Let lesions heal naturally or seek professional extraction if needed.
Q: Do red dots always mean something is wrong?
A: Not at all. Many red dots—like cherry angiomas or keratosis pilaris—are harmless variations of normal skin. Context and accompanying symptoms determine significance.
Final Thought
Most red dots on your skin are nothing to fear—they are simply your body’s way of reacting to life, aging, or minor irritations. But your skin also speaks in details, and the smallest mark can carry the loudest message.
By learning to observe changes with curiosity rather than alarm, you empower yourself to seek care when it truly matters. When in doubt, get it checked. Peace of mind is always worth it, and your health is your most valuable asset.
Listen to your skin. Care for it gently. And trust yourself to know when to reach out for help.